Main Content
Your Wellness Journey Begins at
SIMIO Physical Therapy
Get exceptional care at our physical therapy clinic in Zeeland, MI.
Our Physical Therapy & Wellness Services
Physical Therapy
Measurable results driven by hands-on and exercise programs tailored to your unique needs. Experience a patient-centered, results-oriented physical therapy clinic with consistent one-on-one care. SIMIO offers unmatched personalized care for pain, injury, pre and post-surgery, movement restriction, balance, fitness and sports performance.
Postural Restoration™
Restore your ability to control motion from your center and project power outward toward your limbs. A whole-body approach to wind and unwind with ease. Manage pressure, propulsion, and respiration at the same time and with every step. Breathe easily. Stand or sit effortlessly. SIMIO is the only certified Postural Restoration Center™ in Michigan.
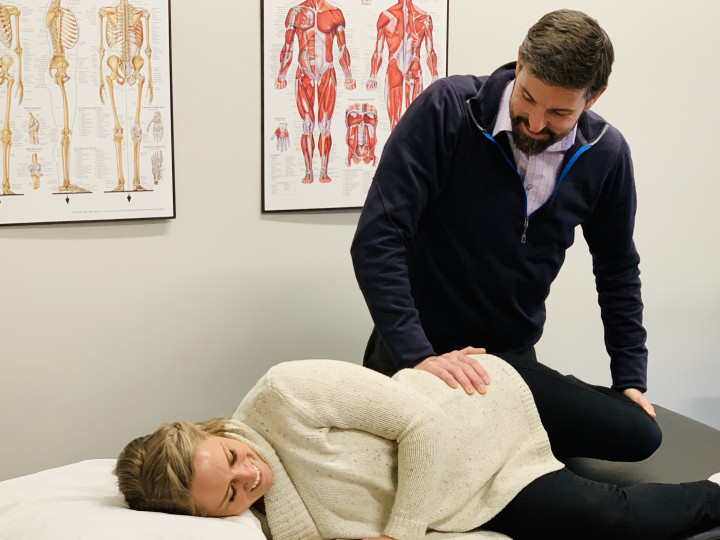
A Hands-on Approach to Physical Therapy and Wellness
We consider the whole body when finding solutions for pain, restricted movement, and sports performance limitations. Guided by a series of unique objective and manual tests, we tailor your care plan to meet your goals. Then, we retest your progress for measurable results.
Our qualifications:
- Our team has over 40 years of combined physical therapy experience
- Our owner is one of the few Postural Restoration (PRI) Certified™ physical therapists in the world and the only certified PRI Provider in Michigan
- Our licensed staff of physical therapists are Doctors of Physical Therapy
Come find wellness at our physical therapy clinic in Zeeland, MI. We're only a short drive from Holland and Grand Rapids, conveniently located just off the Byron Road exit from I-196.
Schedule NowReviews & Testimonials
Meet the Team
Footer
Hours
Mon: 8:00AM-6:00PM
Tue: 8:00AM-6:00PM
Wed: 8:00AM-6:00PM
Thu: 8:00AM-6:00PM
Fri: 8:00AM-1:00PM
Sat: Closed
Sun: Closed
Location
8516 Homestead Drive, Suite 107
Zeeland, MI 49464
Call Us
Phone: (616) 741-9555
Fax: (616) 741-9559